ARVC Specializes in Minimally Invasive Procedures with a Fraction of the Risks and Downtime Compared to Surgery
Click Below to Learn More About the Conditions We Treat
 Osteoarthritis (Joint Pain)
Osteoarthritis (Joint Pain) Sacroiliitis
Sacroiliitis Tendonitis
Tendonitis Uterine Fibroids
Uterine FibroidsAdenomyosis
Benign Prostatic Hyperplasia (BPH)
Hemorrhoids
Plantar Fasciitis
Frozen Shoulder Syndrome
Varicocele
Osteoarthritis Pain Relief at ARV Centers: Advanced, Non-Surgical Solutions
Osteoarthritis (OA), the most common form of arthritis, can significantly impact your quality of life. At ARV Centers, we understand the debilitating effects of joint pain and stiffness. That’s why we offer the most comprehensive, state-of-the-art non-surgical treatments to help you regain mobility and live pain-free.
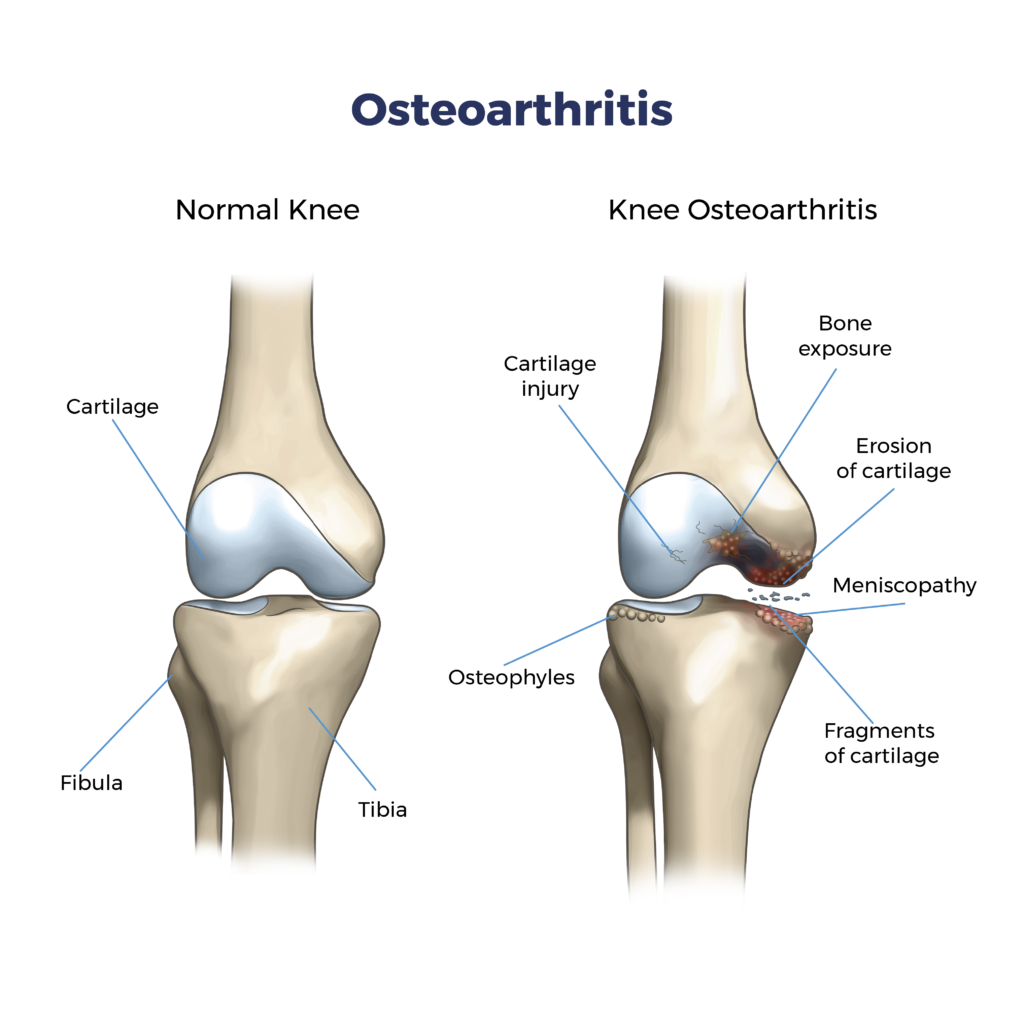
What is Osteoarthritis?
Osteoarthritis is a degenerative joint disease caused by wear and tear on the protective cartilage that cushions the ends of your bones. As cartilage breaks down, bones rub together, leading to pain, inflammation, and reduced joint function. OA most commonly affects weight-bearing joints like the knees, hips, and spine, but can occur in any joint.
- Pain: Often worsens with activity and improves with rest.
- Stiffness: Especially after periods of inactivity.
- Swelling: Around the affected joint.
- Limited Range of Motion: Difficulty moving the joint through its full range.
- Crepitus: A grating or popping sensation in the joint.
We specialize in a range of cutting-edge, minimally invasive treatments to alleviate osteoarthritis pain and restore joint function:
- Intra-articular Steroid Injections: Powerful anti-inflammatory medications delivered directly into the joint to reduce pain and swelling.
- Zilretta for Knee Arthritis: A long-acting corticosteroid injection specifically designed for knee OA.
- Viscosupplementation for Knee Arthritis: Hyaluronic acid injections to lubricate and cushion the knee joint.
- Genicular Artery Embolization (GAE) for Knee Arthritis: A minimally invasive procedure that blocks blood flow to the inflamed lining of the knee joint.
- Shoulder Joint Embolization for Shoulder Arthritis: Similar to GAE, this procedure targets the inflamed lining of the shoulder joint.
- Hip Joint Embolization for Hip Arthritis: A novel treatment option for hip OA that reduces inflammation and pain.
- Regenerative Cellular Therapies: Utilizes your body's natural healing abilities to repair damaged cartilage and promote joint regeneration.
Why Choose ARV Centers for Osteoarthritis Treatment?
- Expertise: Our skilled physicians have extensive experience in diagnosing and treating osteoarthritis using the latest techniques. We have performed hundreds of thousands of joint procedures.
- Comprehensive Approach: We offer a wide array of non-surgical treatment options tailored to your specific needs.
- Minimally Invasive: Our procedures are minimally invasive, meaning less risk, faster recovery with less downtime compared to surgery.
- Focus on Your Quality of Life: We're committed to helping you regain mobility, reduce pain, and improve your overall quality of life.
Take the first step towards a more active, pain-free life. Schedule a consultation with ARV Centers today to discuss your osteoarthritis treatment options.
Sacroiliitis: Find Relief from Pelvic Pain at ARV Centers
Do you experience persistent pain in your lower back, buttocks, or groin? It could be sacroiliitis, a common but often overlooked cause of chronic pain. At ARV Centers, we specialize in diagnosing and treating sacroiliitis, offering a range of non-surgical solutions to help you get back to living your life comfortably.
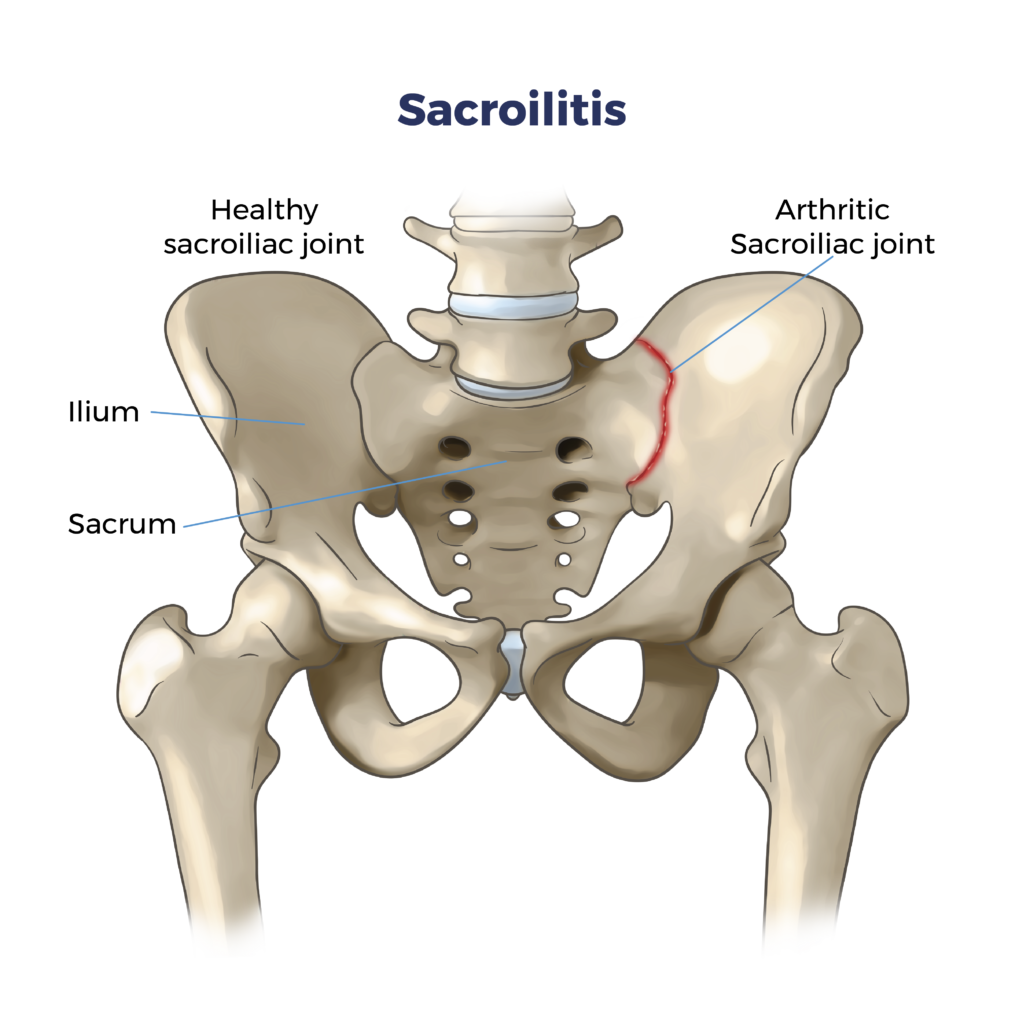
What is Sacroiliitis?
Sacroiliitis is inflammation of the sacroiliac joints, located where your spine connects to your pelvis. These joints play a vital role in supporting your upper body and transferring weight to your legs. When inflamed, they can cause significant pain and discomfort.
- Lower Back Pain: Often described as dull, aching pain that may radiate to the buttocks or groin.
- Stiffness: Difficulty bending or twisting.
- Pain Worsening with Activity: Standing, walking, or climbing stairs can exacerbate pain.
- Pain Improving with Rest: Pain typically lessens when lying down.
- Pain in the Buttocks or Groin: This pain can be sharp or stabbing.
- Injury: A fall, car accident, or repetitive stress can trigger inflammation.
- Arthritis: Inflammatory conditions like ankylosing spondylitis or psoriatic arthritis can affect the sacroiliac joints.
- Pregnancy: Hormonal changes and increased strain on the joints during pregnancy can lead to sacroiliitis.
Advanced Sacroiliitis Treatments at ARV Centers:
We offer several innovative, minimally invasive procedures to target the root cause of sacroiliitis pain:
- Sacroiliac Joint Injections: These injections deliver anti-inflammatory medication directly to the affected joint, providing rapid pain relief.
- Radiofrequency Ablation (RFA): This procedure uses heat to disrupt the nerve fibers that transmit pain signals from the sacroiliac joint.
- Prolotherapy: This regenerative therapy involves injecting a solution that stimulates the body's natural healing response to strengthen and repair the joint.
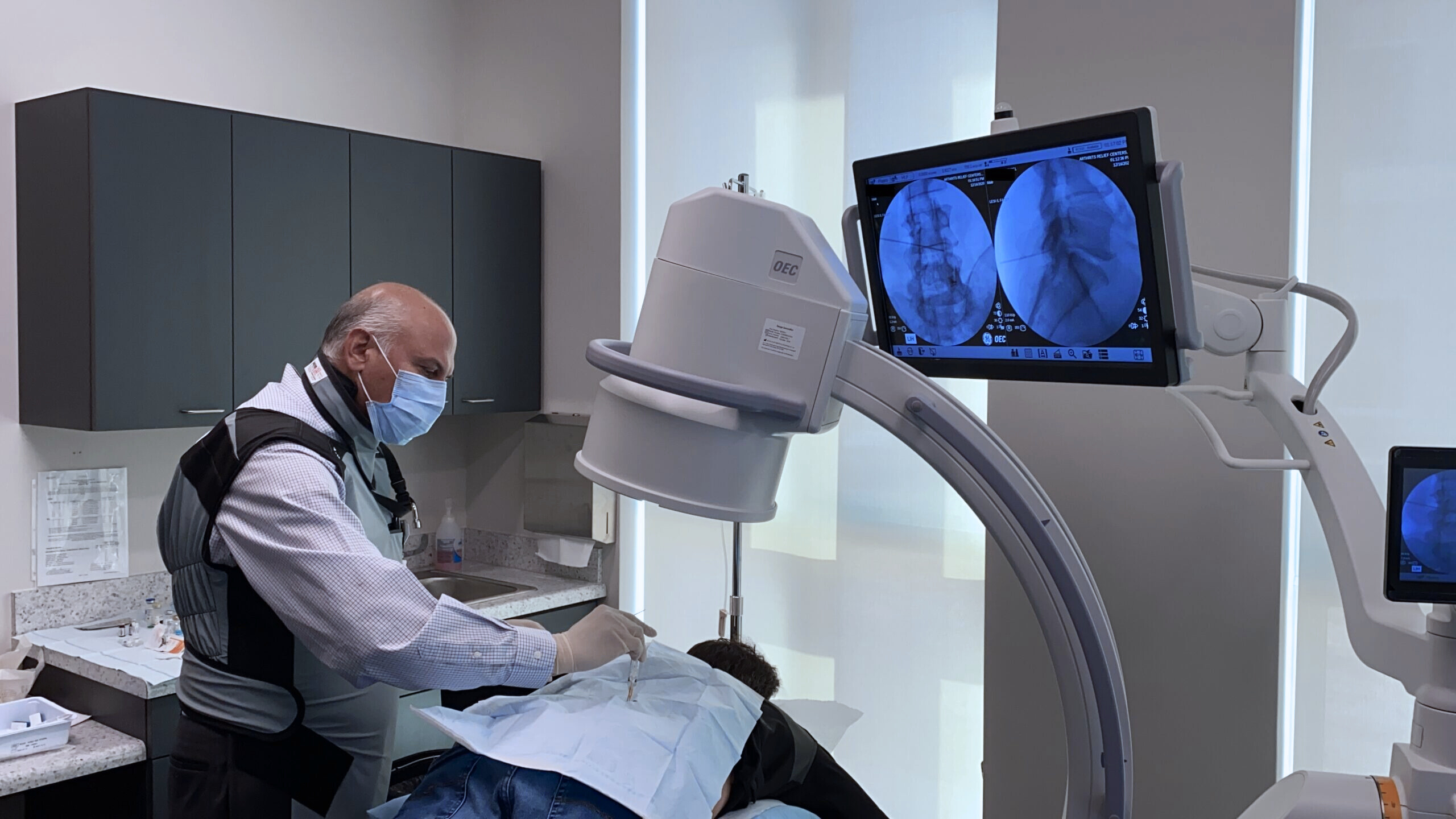
Why Choose ARV Centers for Sacroiliitis Treatment?
- Expert Diagnosis: Our experienced physicians use a multi-faceted approach to accurately diagnose sacroiliitis, including physical exams, medical history review, and imaging studies.
- Personalized Treatment Plans: We tailor treatment to your individual needs and preferences, ensuring the most effective pain relief solution.
- Minimally Invasive: Our procedures are performed with minimal risk and recovery time, allowing you to quickly resume your daily activities.
- Focus on Your Well-Being: We prioritize your comfort and well-being, offering compassionate care and personalized support throughout your treatment journey.
Don't let sacroiliitis pain control your life. Contact ARV Centers today to schedule a consultation and explore your treatment options.
Tendonitis Relief at ARV Centers: Healing Beyond Pain
If persistent tendon pain is hindering your activities and quality of life, ARV Centers can help. Tendonitis, the inflammation of tendons, can be incredibly frustrating and debilitating. We specialize in providing both traditional and innovative treatment options, including PRP therapy, to reduce inflammation, promote healing, and get you back to doing what you love.
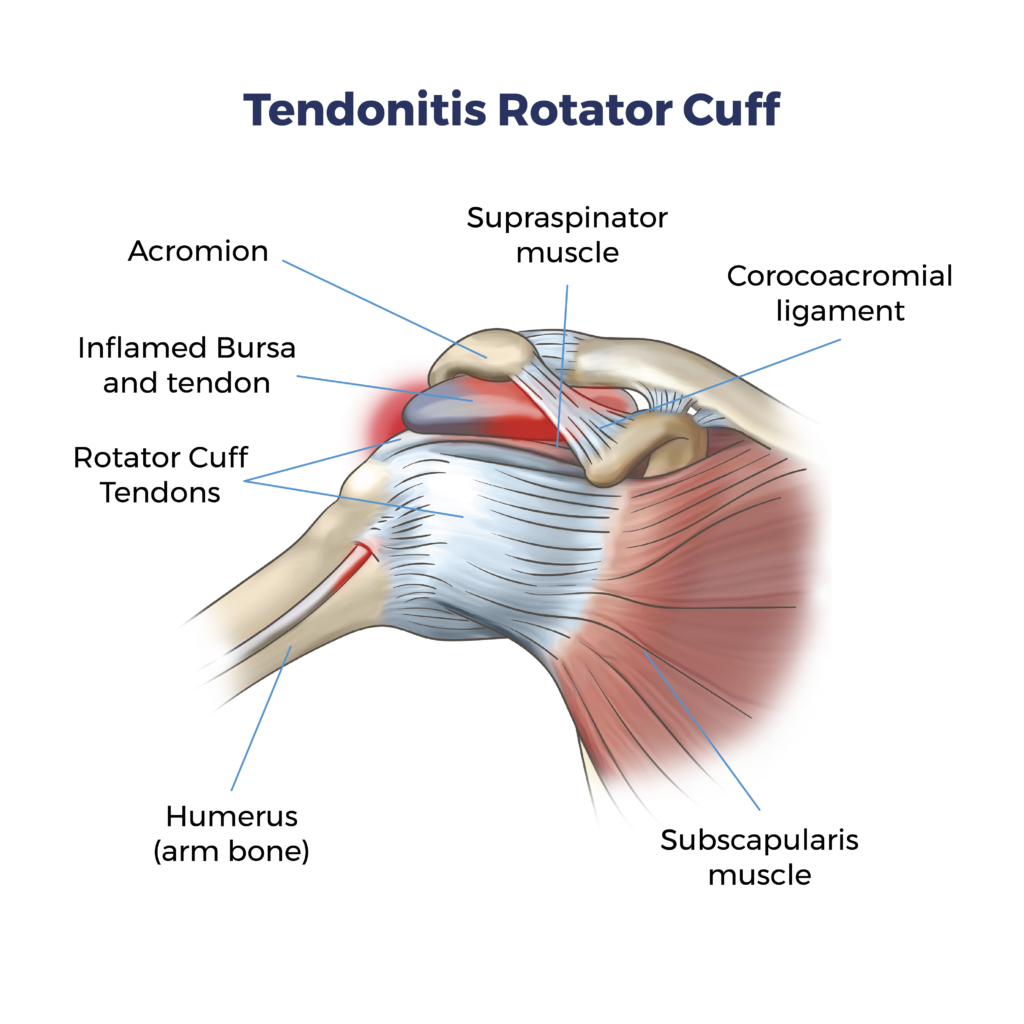
Tendons are tough, fibrous cords that connect muscles to bones. Tendonitis occurs when these tendons become irritated or inflamed, often due to overuse, repetitive motions, or injury. Common areas affected by tendonitis include:
- Shoulder: Rotator cuff tendonitis
- Elbow: Tennis elbow (lateral epicondylitis) or golfer's elbow (medial epicondylitis)
- Wrist and Hand: De Quervain's tenosynovitis
- Knee: Patellar tendonitis (jumper's knee)
- Ankle: Achilles tendonitis
- Pain: Often worsens with movement or activity.
- Tenderness: Discomfort when touching the affected area.
- Swelling: Around the inflamed tendon.
- Stiffness: Difficulty moving the joint connected to the tendon.
We offer a range of proven therapies to address tendonitis and accelerate healing:
- Rest and Activity Modification: Reducing or changing activities that aggravate the tendon is crucial for initial healing.
- Physical Therapy: Specific exercises and stretches can help strengthen the tendon and improve flexibility.
- Steroid Injections: Corticosteroids can be injected into the affected area to reduce inflammation and provide pain relief.
- Platelet-Rich Plasma (PRP) Therapy: This innovative treatment utilizes your own blood's platelets, which contain growth factors that promote healing. PRP injections can stimulate tissue repair and reduce pain.
- Other Options: We may also recommend bracing, taping, or other modalities depending on your individual needs.
Why Choose ARV Centers for Tendonitis Treatment?
- Expert Diagnosis: Our skilled physicians accurately diagnose tendonitis and assess the severity of your condition.
- Personalized Treatment Plans: We create tailored treatment programs based on your unique needs and goals.
- Advanced Therapies: We offer both traditional and cutting-edge options like PRP therapy to optimize healing and recovery.
- Focus on Long-Term Relief: Our goal is not just to alleviate pain but to help you restore function and prevent future tendon problems.
Don't let tendonitis sideline you. Schedule a consultation with ARV Centers today and experience our comprehensive approach to pain relief and faster healing.
Uterine Fibroids? Reclaim Your Life with UFE at ARV Centers
Are uterine fibroids causing pain, heavy bleeding, fatigue or interfering with your daily life? You’re not alone. Millions of women face the challenges of these non-cancerous growths. But at ARV Centers, we offer a proven, minimally invasive solution: Uterine Fibroid Embolization (UFE).
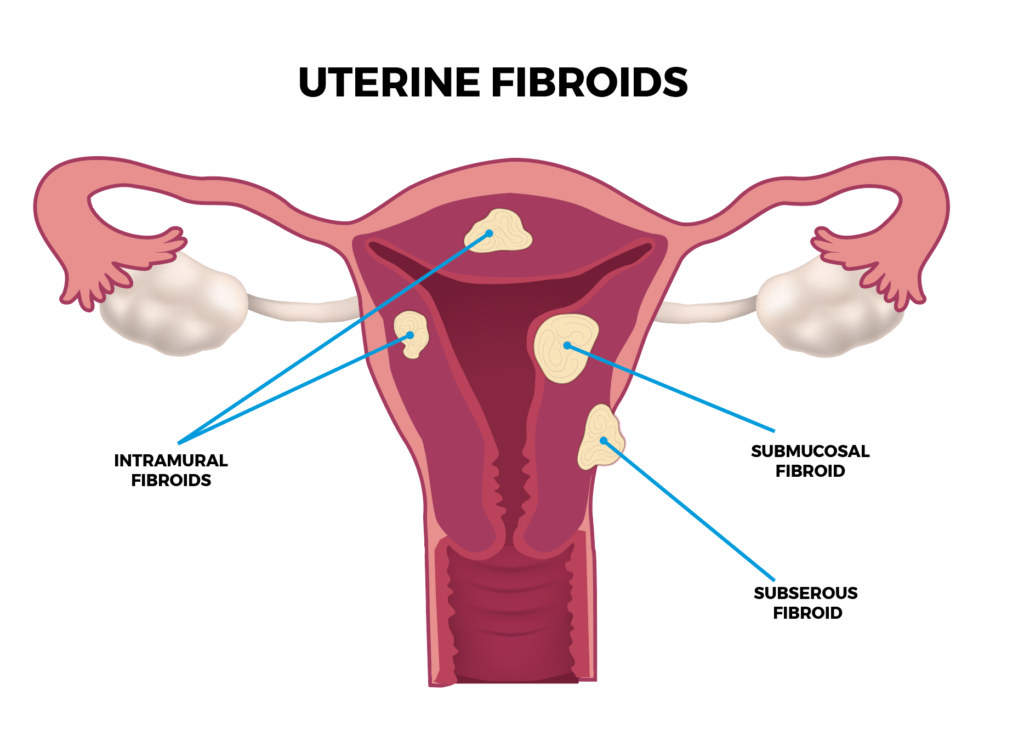
- Heavy or Prolonged Menstrual Bleeding: This can lead to anemia and fatigue.
- Painful Periods: Cramping or aching in the lower abdomen or back.
- Pelvic Pressure or Pain: A feeling of fullness or discomfort in the pelvis.
- Frequent Urination: If fibroids press on the bladder
- Constipation: If fibroids press on the rectum.
- Enlarged Abdomen: In some cases, fibroids can make your belly look larger.
- Pain During Intercourse: Fibroids can sometimes cause discomfort during sexual activity.
The exact cause of fibroids is unknown, but they are believed to be influenced by:
- Hormones: Estrogen and progesterone, the hormones that stimulate the uterine lining to thicken during each menstrual cycle, appear to promote fibroid growth.
- Genetics: Having a family history of fibroids increases your risk.
- Other Factors: Age, race (African-American women are at higher risk), and obesity may play a role.
- Diet: Foods like red meat and alcohol consumption have been linked to fibroids.
Fibroids are often discovered during with the following tests:
- Ultrasound: This imaging test uses sound waves to create a picture of your uterus and identify fibroids.
- MRI (Magnetic Resonance Imaging): This test provides detailed images of the uterus and fibroids, helping to determine their size and location.
- CT: This imaging test is sometimes performed in the setting of an Emergency Room visit if you are complaining of lower abdominal pain. CT is better for visualizing the intestines and for diagnosing more life threatening conditions.
If fibroids are causing symptoms, various treatment options are available:
- Medication: Hormonal medications can help shrink fibroids and reduce symptoms.
- Myomectomy: This surgical procedure removes fibroids while preserving the uterus.
- Hysterectomy: This surgery involves removing the entire uterus.
- Uterine Fibroid Embolization (UFE): This minimally invasive procedure shrinks fibroids by blocking their blood supply.
Why Choose ARV Centers for UFE?
At ARV Centers, we specialize in UFE, a safe and effective alternative to surgery that offers a significantly faster recovery with a fraction of the risks.
Remember: If you're experiencing any symptoms that you think could be related to fibroids, don't wait to schedule a consultation. There are a number of conditions that cause symptoms similar to uterine fibroids and early detection is crucial to a successful treatment outcome.
Understanding Adenomyosis: Causes, Symptoms, and Treatment Options

- Heavy or prolonged menstrual bleeding
- Severe menstrual cramps
- Painful intercourse
- Chronic pelvic pain
- Enlarged or tender uterus
These symptoms often mimic the same symptoms of uterine fibroids, but is somewhat less common and thus most women have never heard of it, much less the treatment options to resolve the symptoms.
- Age: Adenomyosis is most commonly diagnosed in women between the ages of 40 and 50, who are in their late reproductive years.
- Childbirth: You'll receive instructions on fasting and medication schedules after the procedure.
- Prior Uterine Surgeries: Any procedure that involves disruption of the uterine lining, such as a cesarean section, dilation and curettage (D&C), or myomectomy (fibroid removal), can increase the risk.
- Genetics: There's some evidence to suggest that adenomyosis may have a genetic component, as it can sometimes run in families.
- Other Factors: Additional factors that might play a role include early onset of menstruation, short menstrual cycles, endometriosis, uterine fibroids, obesity, and use of certain hormonal medications.
It's important to note that having one or more of these risk factors doesn't guarantee that a woman will develop adenomyosis. Conversely, women without any apparent risk factors can still be affected. If you're concerned about your risk or experiencing symptoms like heavy menstrual bleeding, painful periods, or pelvic pain, it's important to consult with your healthcare provider for proper evaluation and diagnosis.
The optimal treatment for adenomyosis depends on the severity of your symptoms, your desire for future fertility, and your overall health. Options include:
- Pain medication and hormonal therapies: To manage symptoms, doctors may recommend over-the-counter pain relievers, hormonal birth control, or a hormonal intrauterine device (IUD).
- Hysterectomy: Surgical removal of the uterus is the only definitive cure for adenomyosis. However, it eliminates the possibility of future pregnancies.
- Uterine Artery Embolization (UAE): A minimally invasive procedure that blocks the blood supply to the affected areas of the uterus, causing the abnormal tissue to shrink. This can significantly reduce symptoms while preserving the uterus.
At ARV Centers, we specialize in Uterine Artery Embolization (UAE). Our experienced Vascular & Interventional Radiologists utilize advanced imaging techniques to perform UAE with precision and minimal discomfort. This procedure offers a safe and effective alternative to hysterectomy for women seeking relief from adenomyosis without sacrificing their uterus.
Benefits of UAE:
- Minimally invasive: Performed through a tiny incision in the groin.
- Shorter recovery time: Most women return to normal activities within a week.
- Preserves fertility: Maintains the possibility of future pregnancies.
- High success rate: Significant reduction in symptoms for most patients.

Why Choose ARV Centers for UAE?
If you are experiencing symptoms of adenomyosis, schedule a consultation with our experts at ARV Centers. We will thoroughly evaluate your condition and discuss the most suitable treatment options, including UAE. Our goal is to help you regain control of your life and enjoy a symptom-free future.
Remember, you don't have to live with the symptoms of adenomyosis. Effective treatment options are available.
Benign Prostatic Hyperplasia (BPH): Understanding the Condition and Exploring Treatment Options at ARV Centers
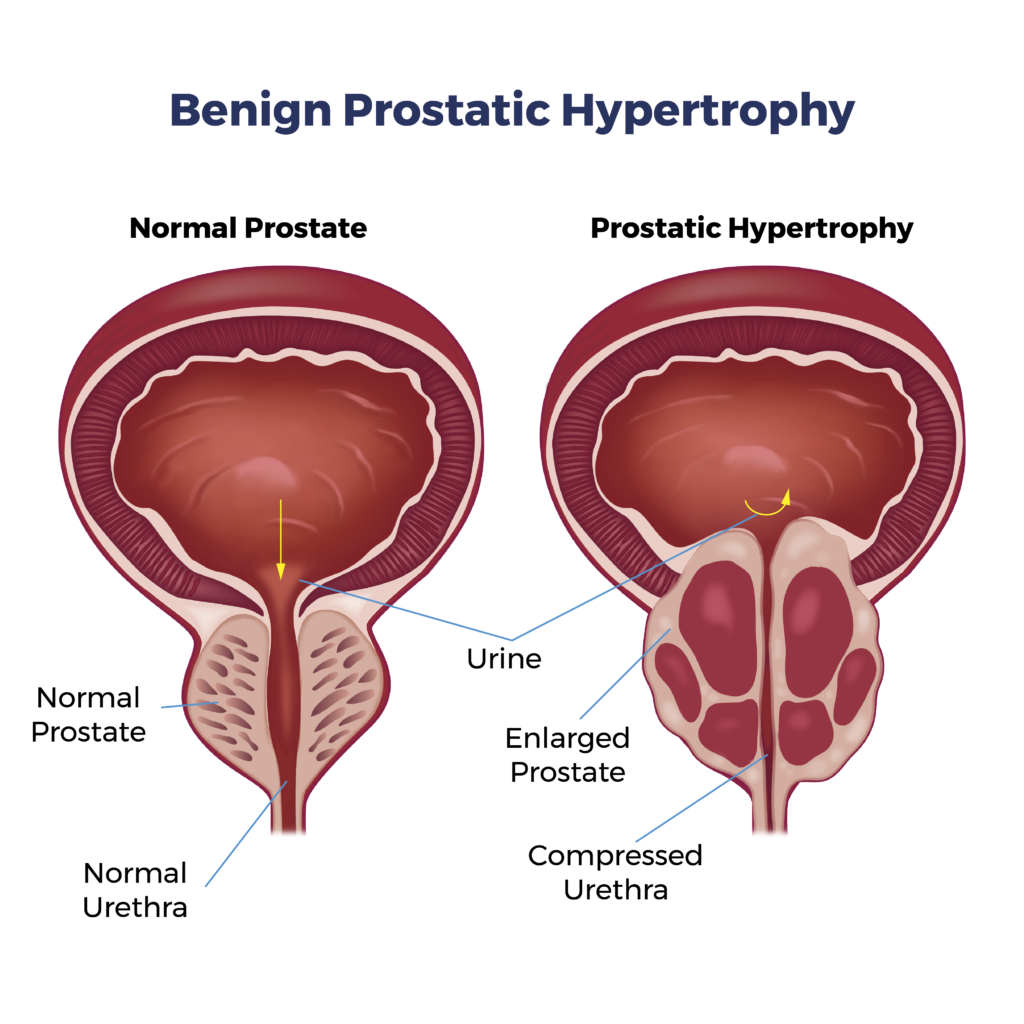
BPH occurs when the prostate gland, located just below the bladder, grows larger than normal. This enlargement can press on the urethra, the tube that carries urine from the bladder out of the body, causing various urinary problems, such as:
- Frequent urination, especially at night (nocturia)
- Urgent need to urinate
- Weak or slow urine stream
- Difficulty starting urination
- Dribbling after urination
- Feeling of incomplete bladder emptying
FEATURED RESOURCE - FREE E-BOOK
A Comprehensive Guide To Prostate Health

Causes and Risk Factors
The exact cause of BPH remains unknown, but it's believed to be related to hormonal changes associated with aging. Several factors can increase your risk of developing BPH, including:
- Age: The risk of BPH increases with age, particularly after the age of 50.
- Family history: Having a father or brother with BPH increases your risk.
- Medical conditions: Certain conditions like diabetes and heart disease may be associated with an increased risk of BPH.
- Lifestyle: Obesity and lack of physical activity may contribute to BPH.
The treatment for BPH depends on the severity of your symptoms and how much they impact your daily life. Options include:
- Lifestyle changes: Dietary modifications, exercise, and bladder training can help manage mild symptoms.
- Medications: Several medications are available to shrink the prostate or relax the muscles around the bladder neck, improving urine flow.
- Minimally invasive procedures: These include transurethral microwave therapy (TUMT), transurethral needle ablation (TUNA), and water vapor therapy.
- Surgery: Traditional surgical options like transurethral resection of the prostate (TURP) are available for severe cases.
At ARV Centers, we specialize in Prostate Artery Embolization (PAE), a minimally invasive procedure that offers several advantages over traditional surgery:
- Preserves sexual function: Unlike some surgical options, PAE has a low risk of impacting sexual function.
- Faster recovery: You can typically go home the same day and resume normal activities within a few days.
- Lower risk of complications: PAE has a lower risk of complications like bleeding, incontinence, and infection compared to surgery.
- High success rate: PAE effectively reduces BPH symptoms in most patients.

How PAE Works
- A thin catheter is inserted through blood vessel in your groin.
- Using advanced imaging technology, the catheter is guided to the prostate arteries.
- Tiny gelatin particles are injected through the catheter to restrict the blood flow to the prostate.
- The reduced blood supply causes the prostate to shrink, relieving urinary symptoms.
If you're struggling with BPH symptoms, consider PAE at ARV Centers.
Contact us today to schedule a consultation and learn more a more about this FDA-Approved, effective, minimally invasive treatment option.
Hemorrhoids: Understanding, Causes, and Treatment Options at ARV Centers
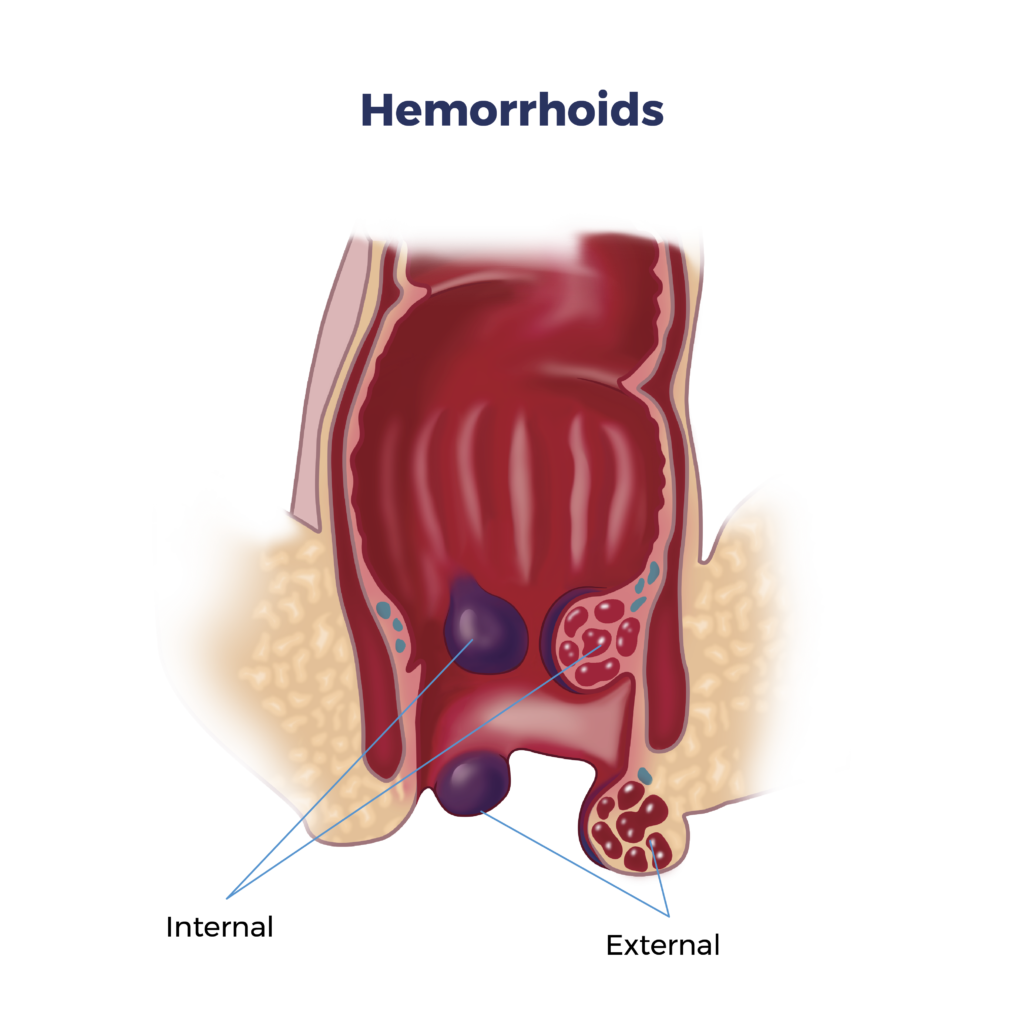
Several factors can contribute to the development of hemorrhoids, including:
- Straining during bowel movements: This is a common cause, often associated with constipation.
- Chronic diarrhea: Can also irritate and inflame the veins in the anal area.
- Pregnancy: The increased pressure in the abdomen during pregnancy can lead to hemorrhoids.
- Obesity: Being overweight or obese can put extra pressure on the veins in the pelvic and rectal area.
- Aging: As we age, the tissues that support the veins in the rectum and anus can weaken, making hemorrhoids more likely.
- Sitting for long periods: This can increase pressure on the veins in the anal area.
- Bleeding: Bright red blood on toilet paper, in the stool, or in the toilet bowl after a bowel movement is a common sign, especially with internal hemorrhoids.
- Itching or irritation: The anal area may feel itchy or irritated, particularly with external hemorrhoids.
- Pain or discomfort: This can range from mild discomfort to severe pain, especially during bowel movements or when sitting.
- Swelling or lump: You may notice a swollen or tender lump near the anus, which could be a thrombosed (clotted) external hemorrhoid.
- Prolapse: In some cases, internal hemorrhoids may protrude through the anus, causing additional pain and discomfort.
The treatment for BPH depends on the severity of your symptoms and how much they impact your daily life. Options include:
- Lifestyle changes: Increasing fiber intake, drinking plenty of fluids, and avoiding straining can help prevent and relieve hemorrhoid symptoms.
- Over-the-counter medications: Creams, ointments, and suppositories can provide temporary relief from pain and itching.
- Minimally invasive procedures: These include rubber band ligation, sclerotherapy, and infrared coagulation, which are typically effective for mild to moderate hemorrhoids.
For more severe or persistent hemorrhoids, ARV Centers specializes in Hemorrhoid Artery Embolization (HAE), a minimally invasive procedure that offers several advantages over traditional surgical options
- A thin catheter is inserted through a small puncture in the groin.
- Using advanced imaging technology, the catheter is guided to the arteries supplying the hemorrhoids.
- Tiny gelatin particles about the size of a grain of sand are injected through the catheter to restrict the blood flow to the hemorrhoids.
- This causes the hemorrhoids to shrink and eventually disappear.
Benefits of HAE
- Minimally invasive: Performed with a small incision and no stitches.
- Less pain: Compared to traditional hemorrhoid surgery.
- Faster recovery: Most patients can return to normal activities within 1-2 days
- In office procedure: No surgery center visits and no hospital stay.
- High success rate: HAE is effective in treating even severe hemorrhoids.
If you're struggling with hemorrhoids, don't suffer in silence. Contact ARV Centers today to learn more about HAE and how we can help you find relief.
Plantar Fasciitis: Understanding, Causes, Symptoms, and Treatment Options at ARV Centers
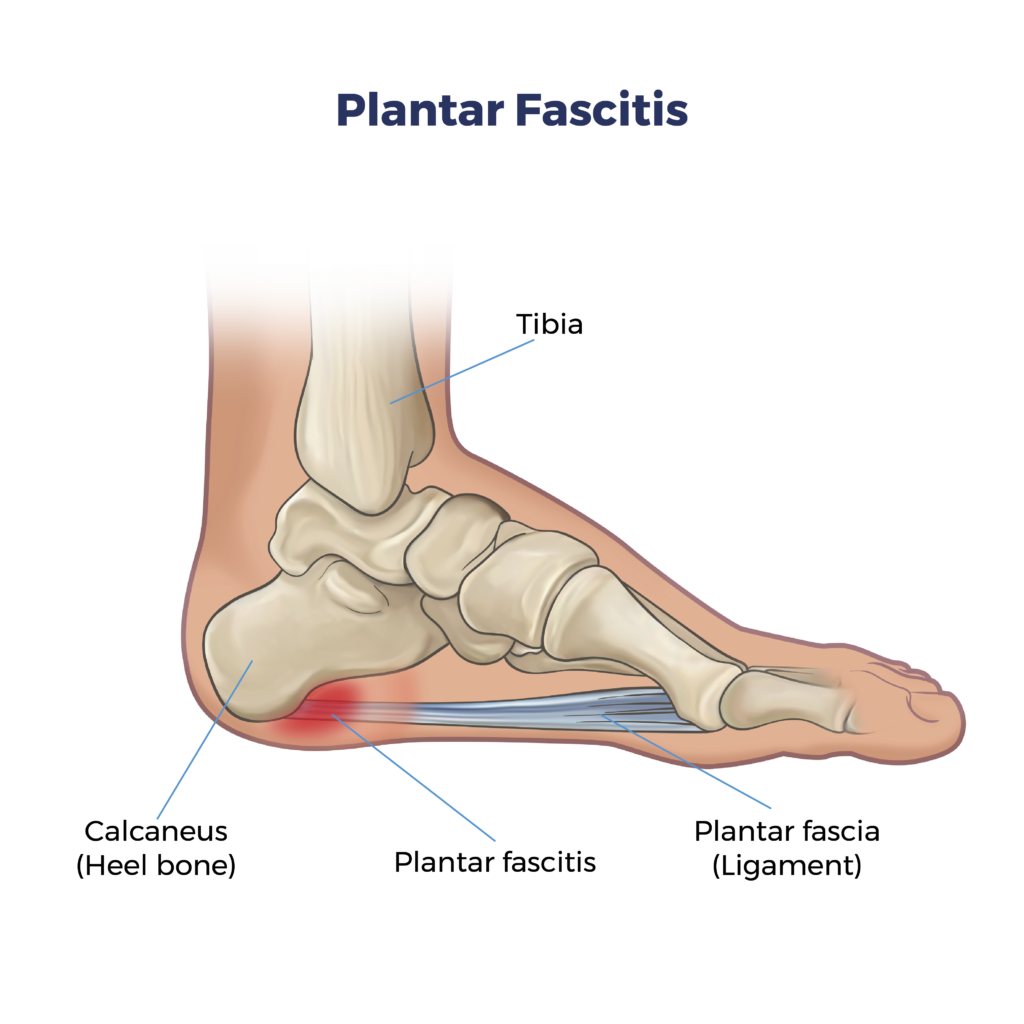
The plantar fascia acts as a shock absorber and supports the arch of your foot. When it becomes overstressed or strained, tiny tears can develop in the fascia, leading to inflammation and pain. This pain is typically most noticeable in the morning or after periods of rest, and it may worsen with prolonged standing or activity.
The primary symptom of plantar fasciitis is:
- Heel Pain: Often described as a sharp or stabbing pain, it's usually felt on the bottom of the heel or along the arch of the foot. The pain is typically worse in the morning or after periods of rest and may improve with gentle activity.
Other symptoms may include:
- Stiffness in the foot
- Tenderness or swelling in the heel
- Difficulty walking or standing for long periods
Several factors can contribute to the development of plantar fasciitis, including:
- Overuse or repetitive strain: Activities like running, jumping, or standing for long periods can put excessive stress on the plantar fascia.
- Foot structure: Flat feet, high arches, or tight Achilles tendons can increase the risk.
- Obesity: Excess weight puts additional strain on the feet.
- Age: Plantar fasciitis is more common in people between the ages of 40 and 60.
- Certain occupations: Jobs that require prolonged standing or walking on hard surfaces can increase the risk.
At ARV Centers, we offer a comprehensive approach to treating plantar fasciitis. We will work with you to develop a personalized treatment plan tailored to your specific needs and the severity of your condition. Treatment options may include:
- Physical Therapy: Specific exercises and stretches to strengthen and stretch the plantar fascia and surrounding muscles.
- Custom Orthotics: Shoe inserts to provide support and correct any biomechanical imbalances.
- Medications: Over-the-counter or prescription pain relievers or anti-inflammatory medications to manage pain and reduce inflammation.
- Steroid Injections: Corticosteroid injections to reduce inflammation and provide pain relief.
- PRP: Platelet Rich Plasma injections to reduce inflammation and provide pain relief.
- Extracorporeal Shock Wave Therapy (ESWT): A non-invasive treatment that uses sound waves to stimulate healing and reduce pain.
If you've tried conservative treatments like physical therapy and injections without success, Plantar Fascia Embolization (PFE) may be an effective solution. PFE is a minimally invasive procedure that targets the source of inflammation and pain in the plantar fascia.
At ARV Centers, we offer a comprehensive approach to treating plantar fasciitis. We will work with you to develop a personalized treatment plan tailored to your specific needs and the severity of your condition. Treatment options may include:
- Minimally Invasive: Performed with a small puncture and local anesthetic.
- Quick Recovery: Most patients can walk immediately after the procedure and return to normal activities within a few days.
- High Success Rate: Significant pain relief and improved function in most patients.
At ARV Centers, we offer a comprehensive approach to treating plantar fasciitis. We will work with you to develop a personalized treatment plan tailored to your specific needs and the severity of your condition. Treatment options may include:
- A thin catheter is inserted through a small incision in the groin or ankle.
- Using X-ray guidance, the catheter is navigated to the small arteries feeding the inflamed plantar fascia.
- Temporary embolic agents like antibiotic foams are injected through the catheter to restrict the blood flow to the inflamed area.
- This reduces inflammation and promotes healing of the plantar fascia.

Why Choose ARV Centers for PFE?
If you're struggling with the pain and limitations of plantar fasciitis, contact ARV Centers today to learn more about our treatment options, including Plantar Fascia Embolization.
Our team of experts will work with you to develop a personalized treatment plan to help you get back on your feet and enjoy a pain-free life.
Frozen Shoulder Syndrome: Understanding, Causes, Symptoms, and Treatment Options at ARV Centers
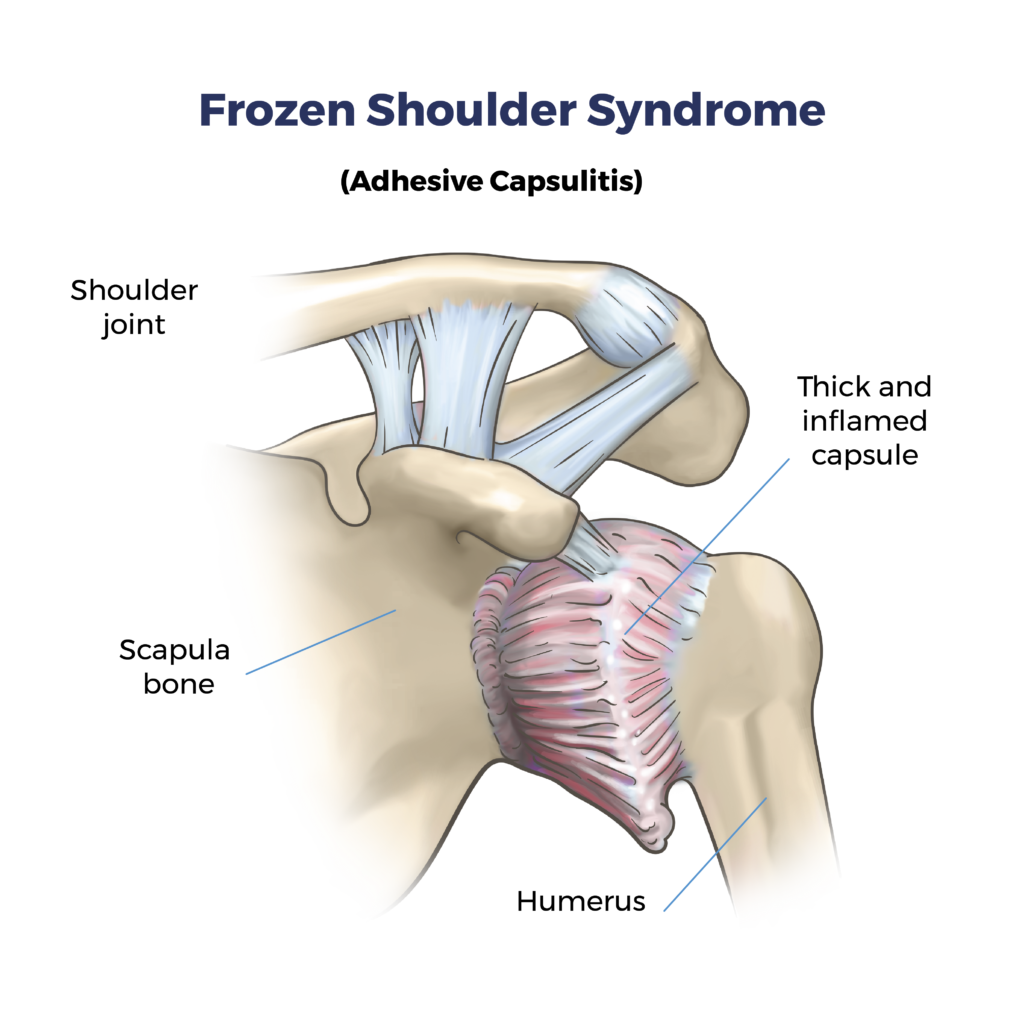
Frozen shoulder occurs when the capsule surrounding the shoulder joint becomes inflamed and thickens, leading to scarring and adhesions that restrict movement. This condition typically progresses through three stages:
- Freezing Stage: Characterized by increasing pain and stiffness, making it difficult to move the shoulder.
- Frozen Stage: Pain may subside, but stiffness and limited range of motion persist.
- Thawing Stage: The shoulder gradually begins to regain its mobility.
The primary symptoms of frozen shoulder include:
- Pain: Often a dull or aching pain, which can be severe at night or when trying to move the shoulder.
- Stiffness: Difficulty moving the shoulder, impacting your ability to perform daily tasks like reaching or dressing.
- Limited range of motion: Significant reduction in the shoulder's ability to rotate and move in various directions.
While the exact cause remains unknown, certain factors can increase your risk of developing frozen shoulder, including:
- Age: Most common in people between 40 and 60 years old.
- Gender: Women are more likely to develop frozen shoulder than men.
- Immobilization: Prolonged immobility of the shoulder, such as after an injury or surgery, can increase the risk.
- Underlying Medical Conditions: Diabetes, thyroid problems, and other systemic diseases can contribute to the development of frozen shoulder.
At ARV Centers, we believe in a comprehensive approach to treating frozen shoulder. We offer a range of treatment options tailored to your specific needs and severity of your condition, including:
- Physical Therapy: Exercises and stretches to improve shoulder mobility and flexibility.
- Medications: Pain relievers and anti-inflammatory medications to manage pain and reduce inflammation.
- Steroid Injections: Corticosteroid injections into the shoulder joint to provide pain relief and reduce inflammation.
- Shoulder Joint Embolization: A minimally invasive, in-office procedure that targets the angiogenic network of blood vessels and nerves responsible for the chronic pain, offering significant relief and improved function for patients who have not responded to other treatments.
If you've tried physical therapy and injections without success, shoulder joint embolization may be the solution you're looking for. After a period of time when the joint pain becomes chronic, the synovial membrane will begin to develop an accessory network of blood vessels and nerve endings called angiogenesis. This process is responsible for the perpetual vicious cycle of pain leading to more inflammation and leading to more pain. Shoulder joint embolization treats the angiogenesis by injecting small gelatin particles through specific blood vessels in the shoulder joint, about the size of grains of sand, to block blood flow to the excess vessels and nerves offering significant pain relief and improved range of motion.
- Minimally invasive: Performed in-office with a small puncture into the wrist after local anesthesia and twilight sedation.
- Quick recovery: Most patients can return to their normal activities within a few days.
- High success rate: Significant pain relief and improved function in most patients.
At ARV Centers, we offer a comprehensive approach to treating plantar fasciitis. We will work with you to develop a personalized treatment plan tailored to your specific needs and the severity of your condition. Treatment options may include:
- A thin catheter is inserted through a small incision in the groin or ankle.
- Using X-ray guidance, the catheter is navigated to the small arteries feeding the inflamed plantar fascia.
- Temporary embolic agents like antibiotic foams are injected through the catheter to restrict the blood flow to the inflamed area.
- This reduces inflammation and promotes healing of the plantar fascia.

Why Choose ARV Centers for Shoulder Joint Embolization?
If you're struggling with the pain and limitations of frozen shoulder, contact ARV Centers today to learn more about our treatment options, including shoulder joint embolization. Our team of experts will work with you to develop a personalized treatment plan to help you regain your mobility and quality of life.
Remember, you don't have to live with the pain of frozen shoulder. Effective treatment options are available at ARV Centers.
Varicocele: A Comprehensive Overview and Treatment at ARV Centers
Understanding Varicoceles
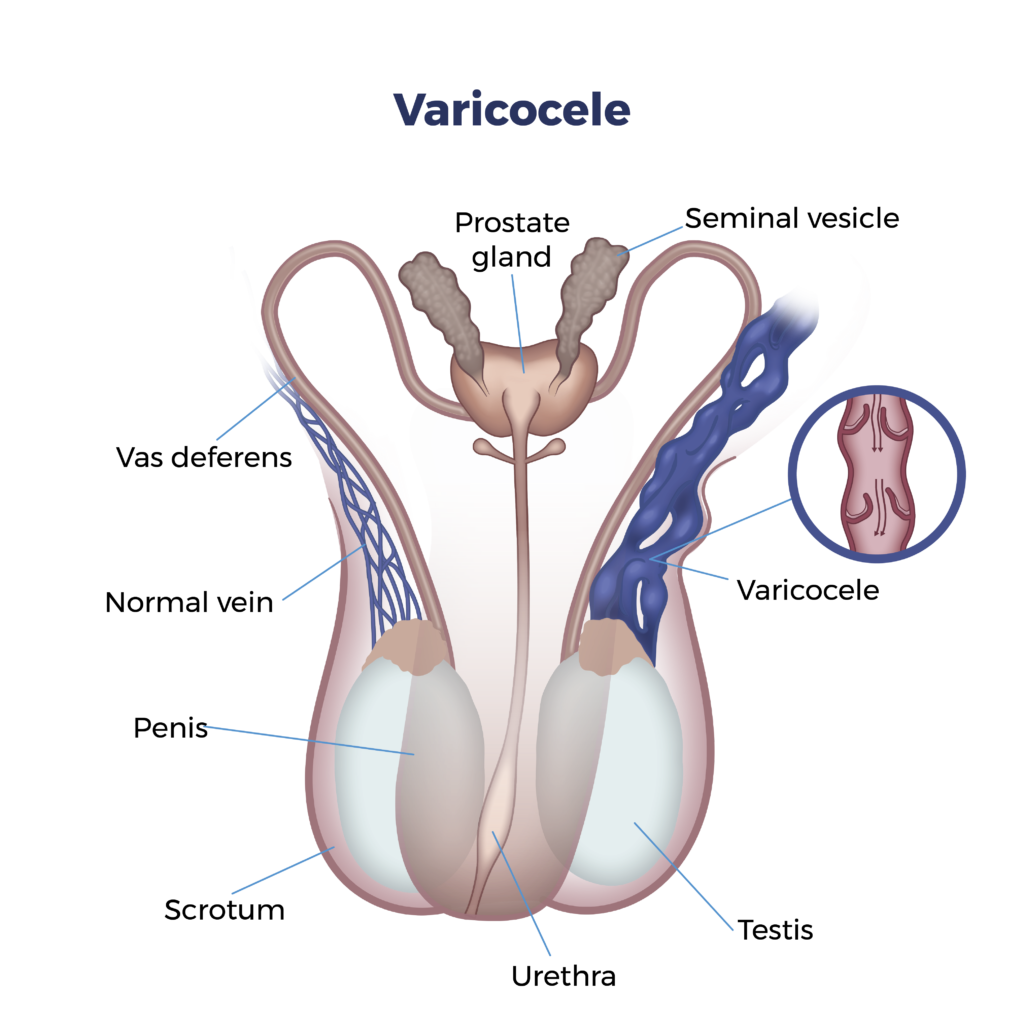
Varicoceles occur when the valves within the veins that carry blood away from the testicles malfunction. This allows blood to pool in the veins, causing them to enlarge. The exact cause of this valve dysfunction is not fully understood, but it's believed to be related to factors such as:
- Anatomy: The left testicular vein is longer and has a less direct path to the heart than the right, making it more susceptible to backflow and varicocele formation.
- Increased Pressure: Activities that increase pressure in the abdomen, such as heavy lifting or straining, can contribute to varicocele development.
- Congenital Abnormalities: In some cases, varicoceles may be present from birth due to abnormalities in the veins.
Many men with varicoceles experience no symptoms at all. However, some may notice:
- Aching or dull pain in the scrotum: This pain may worsen with prolonged standing or physical activity and improve when lying down.
- Visible or palpable enlargement of the veins in the scrotum: The affected veins may feel like a soft, twisted mass.
- Testicular shrinkage or asymmetry: In some cases, the testicle on the affected side may become smaller or feel softer than the other testicle.
- Infertility: Varicoceles can sometimes impair sperm production or quality, leading to difficulties with conception.
If a varicocele is causing pain, testicular shrinkage, or infertility, treatment may be recommended. Treatment options include:
- Observation: If the varicocele is not causing any symptoms or affecting fertility, your doctor may recommend simply monitoring it with regular checkups.
- Surgery: Varicocelectomy is a surgical procedure that involves tying off or removing the affected veins. While effective, it does involve general anesthesia and a longer recovery period.
- Testicular Vein Embolization: At ARV Centers, we specialize in this minimally invasive in-office procedure. It involves inserting a thin catheter through a small puncture in the groin and using X-ray guidance to reach the affected veins. Small coils or a sclerosing agent are then used to block the blood flow, causing the varicocele to shrink.
- Minimally invasive: Performed with a small puncture, resulting no scarring and a significantly faster recovery compared to surgery.
- Local anesthesia/conscious sedation: You'll be awake during the procedure but comfortable with local anesthesia and “twilight” sedation.
- Quick recovery: Most patients can return to normal activities within 1-2 days.
- High success rate: Testicular vein embolization is highly effective in reducing varicocele size and improving symptoms, with success rates comparable to surgery.
- Expert care: Our experienced Vascular & Interventional Radiologists specialize in performing this procedure with precision and expertise.

Why Choose ARV Centers for Testicular Vein Embolization?
If you're experiencing symptoms of a varicocele or concerned about its impact on your fertility, consider testicular vein embolization at ARV Centers. Schedule a consultation today to learn more about this effective, minimally invasive treatment option.


